Replacing missing teeth with durable, natural-looking restorations is both an art and a science. Implant restorations restore chewing function, preserve facial structure, and help patients feel more confident about their smiles. Below you’ll find an in-depth look at what implant restorations involve, how they are planned and placed, and what you can expect from treatment at our practice.
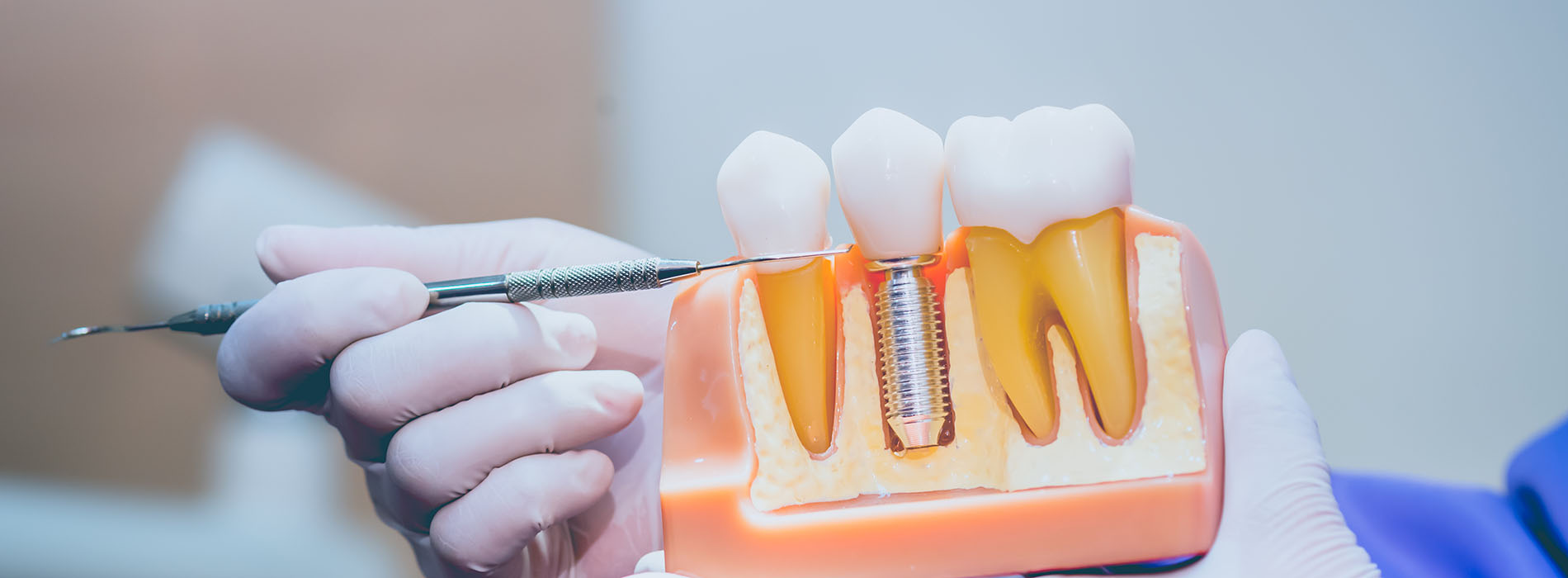
Implant restorations are prosthetic teeth that attach to titanium or ceramic posts surgically placed into the jawbone. Those posts function like artificial tooth roots, anchoring crowns, bridges, or prostheses with a stability that closely mimics natural teeth. Because the restoration is supported by the bone rather than neighboring teeth, it preserves adjacent tooth structure and helps maintain jawbone volume over time.
Beyond function, modern implant restorations are designed to blend seamlessly with the rest of a patient’s smile. Materials such as high-strength ceramics and advanced porcelain blends are used for color matching and translucency, producing lifelike results. Properly designed restorations also restore proper bite forces, which supports comfortable chewing and long-term oral health.
Another reason implants are preferred is their role in oral biology: when a biocompatible post integrates with the jawbone through a process called osseointegration, the result is a stable foundation that resists movement and provides predictable support for restorations. This combination of biological stability and custom restorative design is the foundation of reliable implant care.
Successful implant restorations begin with careful planning. A comprehensive evaluation includes a clinical exam, imaging to assess bone volume and nerve positions, and a review of overall health factors that influence healing. Digital tools such as CBCT scans and intraoral scans are often used to map the jaw precisely and plan the ideal position for each implant.
Placement is a surgical step performed by a qualified clinician. After the implant is positioned in the bone, a healing period follows to allow osseointegration. Depending on the case, a temporary restoration may be used during this phase to maintain aesthetics and function. Once the implant has integrated, an abutment is attached and impressions are taken to craft the final restoration.
The final restoration — whether a single crown, implant-supported bridge, or a fixed hybrid prosthesis — is custom fabricated to match your bite, color, and tooth anatomy. The restorative dentist fine-tunes occlusion and contours to ensure comfort and longevity. Because this is a multidisciplinary process, coordination between surgical and restorative teams is essential to achieve predictable, natural results.
Material selection plays a major role in how natural an implant restoration appears and how it performs. All-ceramic and zirconia restorations are popular choices for their lifelike color and translucency, while layered porcelain can provide nuanced shading for front teeth. For posterior restorations where strength is essential, certain ceramic formulations or metal-ceramic combinations may be used to balance durability and aesthetics.
The design of the restoration takes into account more than just appearance: contours must allow for easy cleaning, proper gum support, and optimal force distribution during chewing. A well-shaped crown or bridge reduces plaque accumulation and protects surrounding tissues. The abutment design — whether stock or custom — also influences the emergence profile and the final look of the restoration at the gum line.
Advanced laboratory techniques and digital workflows enhance accuracy. CAD/CAM design, precise milling, and color-matching technology allow technicians to reproduce natural tooth anatomy with consistent results. These methods also help produce restorations that seat predictably and require minimal adjustment at delivery.
Implant restorations are a reliable option for many patients, including those missing a single tooth, several adjacent teeth, or all teeth in an arch. Ideal candidates have good general health, controlled periodontal (gum) health, and adequate bone volume at the implant site. For individuals with insufficient bone, bone grafting or ridge augmentation procedures can often create a suitable foundation.
Certain medical conditions or habits can affect candidacy and healing. Smoking, uncontrolled diabetes, and active gum disease can increase the risk of complications and should be managed before implant treatment proceeds. A thorough medical and dental history, along with imaging, helps the team develop a treatment plan tailored to each patient’s circumstances.
Age alone is not a limiting factor; the key considerations are oral health, bone condition, and overall medical status. During the consultation, the restorative dentist will explain alternatives, expected outcomes, and any preparatory procedures that may be needed to achieve a successful restoration.
Long-term success of implant restorations depends on consistent home care and professional maintenance. Daily brushing and flossing around the restoration are essential to prevent plaque buildup and maintain healthy soft tissues. Special interdental brushes or floss designed for implant care may be recommended to keep the area clean without damaging the restoration or surrounding gums.
Regular dental visits allow the dental team to monitor implant health, check occlusion, and professionally clean areas that are difficult to reach at home. Routine evaluations also help detect early signs of complications such as peri-implant mucositis or peri-implantitis so they can be addressed promptly. In some cases, a nightguard may be advised for patients who clench or grind their teeth to protect the restoration from excess forces.
With appropriate care and regular professional attention, implant restorations can provide years of reliable function and aesthetics. Factors that influence longevity include material choice, bite dynamics, oral hygiene, and timely management of any issues that arise. Your restorative team will outline a maintenance schedule tailored to your needs and the specifics of your restoration.
Implant restorations offer a dependable, natural-looking solution for replacing missing teeth and restoring oral function. Thoughtful planning, careful material selection, and ongoing maintenance are the keys to predictable outcomes. If you would like to learn more about implant restorations or explore whether they are a good option for you, contact Vita Head, Neck & Facial Pain Relief Center for more information.

Implant restorations are prosthetic teeth that attach to a biocompatible post surgically placed in the jaw to replace missing teeth and restore function. These restorations can take the form of single crowns, implant-supported bridges, or full-arch prostheses and are designed to integrate with surrounding bone and soft tissue. Modern materials and lab techniques create lifelike color, shape, and translucency so the restoration blends naturally with adjacent teeth.
Because an implant restoration is supported by bone rather than neighboring teeth, it preserves adjacent tooth structure and helps maintain jawbone volume over time. Properly designed restorations also restore bite forces and chewing efficiency, which supports comfortable function and long-term oral health. The goal of treatment is predictable comfort, stability, and an appearance that complements the rest of the smile.
The process begins with a comprehensive evaluation that typically includes a clinical exam, dental imaging such as CBCT, and a review of medical history to plan implant position and assess bone volume. A qualified clinician places the implant post in the jaw and a healing period follows to allow biological integration with the bone, during which a temporary restoration may be used for aesthetics and function. After integration, an abutment is attached and impressions or digital scans are taken to fabricate the final crown, bridge, or prosthesis.
The final restoration is custom-designed to match tooth anatomy, bite relationships, and gum contours so it fits comfortably and functions predictably. Occlusion and contours are fine-tuned at delivery to minimize adjustments and reduce long-term wear. Coordination between surgical and restorative clinicians ensures that each step supports the desired aesthetic and functional outcome.
Osseointegration is the biological process by which bone grows tightly around a biocompatible implant surface, creating a stable foundation similar to a natural tooth root. This direct bone-to-implant contact is essential for preventing micromovement and ensuring the long-term stability of the restoration under chewing forces. The quality of osseointegration affects how soon a restoration can be loaded and how reliably it will perform over time.
Factors that influence osseointegration include bone quality and quantity, the implant surface design, and the patient’s systemic health and habits. A careful surgical technique and appropriate healing period allow predictable integration in most cases. When integration is successful, it provides the mechanical support needed for durable and comfortable restorations.
Many patients who are missing one or more teeth can be considered for implant restorations, provided they have adequate bone volume and controlled periodontal health. Good general health, proper oral hygiene, and realistic expectations are important considerations when determining candidacy. Age alone is not a disqualifying factor; the key elements are tissue health, bone condition, and medical factors that affect healing.
Certain conditions or habits—such as uncontrolled diabetes, active gum disease, or heavy smoking—can increase the risk of complications and should be managed before implant treatment proceeds. When bone is insufficient, grafting or ridge augmentation procedures can often create a strong foundation for implants. A thorough consultation and imaging help the dental team develop a personalized plan that addresses individual needs and risk factors.
Advanced laboratory workflows and CAD/CAM milling allow precise fit and consistent color matching, reducing chairside adjustments at delivery. Technicians can layer porcelain or stain ceramic surfaces to reproduce natural shading and texture for anterior restorations. Material selection is guided by location in the mouth, opposing dentition, and the patient’s functional demands to balance durability and appearance.
Bone grafting or sinus lift procedures are considered when the native jawbone lacks sufficient height or width to support stable implant placement. Common reasons for bone deficiency include long-term tooth loss, periodontal disease, or anatomic limitations such as a low sinus floor in the upper jaw. Grafting options range from socket preservation and ridge augmentation to block grafts and lateral or crestal sinus elevation, chosen based on the specific defect.
These preparatory procedures aim to recreate adequate bone volume so implants can achieve primary stability and osseointegration. Healing timelines vary by graft type and patient factors, and the restorative plan is adjusted to accommodate the staged approach when necessary. With appropriate planning, grafting can expand candidacy and improve long-term outcomes for implant-supported restorations.
Initial recovery after implant surgery commonly involves mild swelling, tenderness, and occasional bruising that typically peak within the first 48 to 72 hours and then gradually subside. Pain and discomfort are usually managed with prescribed or over-the-counter medications, and patients are advised to follow a soft diet and avoid strenuous activity for a short period. Maintaining oral hygiene around the surgical site and attending follow-up visits are important to support healing and detect any early issues.
The full osseointegration period can range from a few weeks to several months depending on implant location, bone quality, and systemic health. Temporary restorations may be used during healing to preserve appearance and function while protecting the implant site from excessive forces. Regular post-operative checks allow the team to verify integration and move forward with the final restorative phases at the appropriate time.
Long-term care for implant restorations combines diligent home oral hygiene with regular professional maintenance to prevent plaque-related complications around the implant. Daily brushing and cleaning with implant-safe tools, such as floss designed for implants or interdental brushes, help keep the area free of biofilm and reduce the risk of peri-implant mucositis. Avoiding tobacco and managing systemic health factors also supports tissue health and implant longevity.
Routine dental visits let the clinician monitor occlusion, check the integrity of the restoration, and provide thorough cleaning in areas that are difficult to access at home. In some cases, a protective nightguard may be recommended for patients who brux to reduce excessive forces on the restoration. Prompt attention to any symptoms such as mobility, persistent swelling, or bleeding helps address problems early and preserve the investment in function and aesthetics.
Complications can be biological, such as peri-implant mucositis or peri-implantitis, or mechanical, such as abutment loosening, screw fracture, or porcelain chipping. Risk factors include poor oral hygiene, uncontrolled systemic conditions, smoking, and unfavorable bite forces, and early recognition through regular exams improves the chance of successful intervention. Management ranges from nonsurgical therapy and improved home care to surgical intervention and prosthetic repair depending on the severity of the issue.
Preventive strategies focus on maintenance visits, careful occlusal design, appropriate material selection, and patient education to minimize risk. When complications occur, a coordinated approach between the restorative dentist and surgeon addresses the underlying cause and restores function. Most problems can be managed effectively when detected early and treated promptly.
At Vita Head, Neck & Facial Pain Relief Center the surgical and restorative teams collaborate from the initial consultation to ensure treatment planning, imaging, and prosthetic goals are aligned for each patient. Digital tools such as CBCT imaging and intraoral scanning are often used to plan implant position, design surgical guides, and communicate exact restorative requirements to the laboratory. This coordinated workflow helps place implants in positions that support long-term aesthetics, hygiene access, and occlusal stability.
Patient education and staged appointments are part of the process so expectations are clear and each phase proceeds on a predictable timeline. Clear communication between clinicians, technicians, and the patient allows timely adjustments if additional procedures such as grafting are needed. The result is a personalized plan that prioritizes functional success, tissue health, and a natural appearance.

We’re here to answer your questions and help you take the next step toward relief.
Have questions about your symptoms, treatment options, or scheduling an appointment? Our friendly and knowledgeable team is always happy to assist you. Whether you’re seeking relief from TMJ disorders, head and neck pain, facial discomfort, or general dental concerns, we take the time to listen and provide clear, thoughtful answers. From your first call to your ongoing care, we are committed to offering personalized support, helping you understand your options, and guiding you toward lasting comfort, improved function, and exceptional care.