Tooth loss affects people in many ways — from the practical challenge of chewing to the quieter, personal impact on self-image. Modern implant dentistry addresses those concerns by restoring both function and appearance in a way that feels natural. Rather than relying on removable appliances or altering adjacent teeth, implants recreate the missing tooth structure from root to crown, giving patients a durable and comfortable option for rebuilding their smiles.
Implants are appropriate for a wide range of situations: a single missing tooth, several gaps in a row, or total arch replacement. The goal is consistent across cases — to return reliable bite force, preserve surrounding bone, and provide a long-term foundation for a lifelike restoration. For many people, this means regaining the confidence to eat, speak, and smile without constant worry.
Our team at Vita Head, Neck & Facial Pain Relief Center approaches implant care with an emphasis on precision and patient comfort. We take time to explain the process, evaluate individual needs with detailed imaging, and develop a plan that balances predictable outcomes with an aesthetic result that suits each patient’s face and lifestyle.
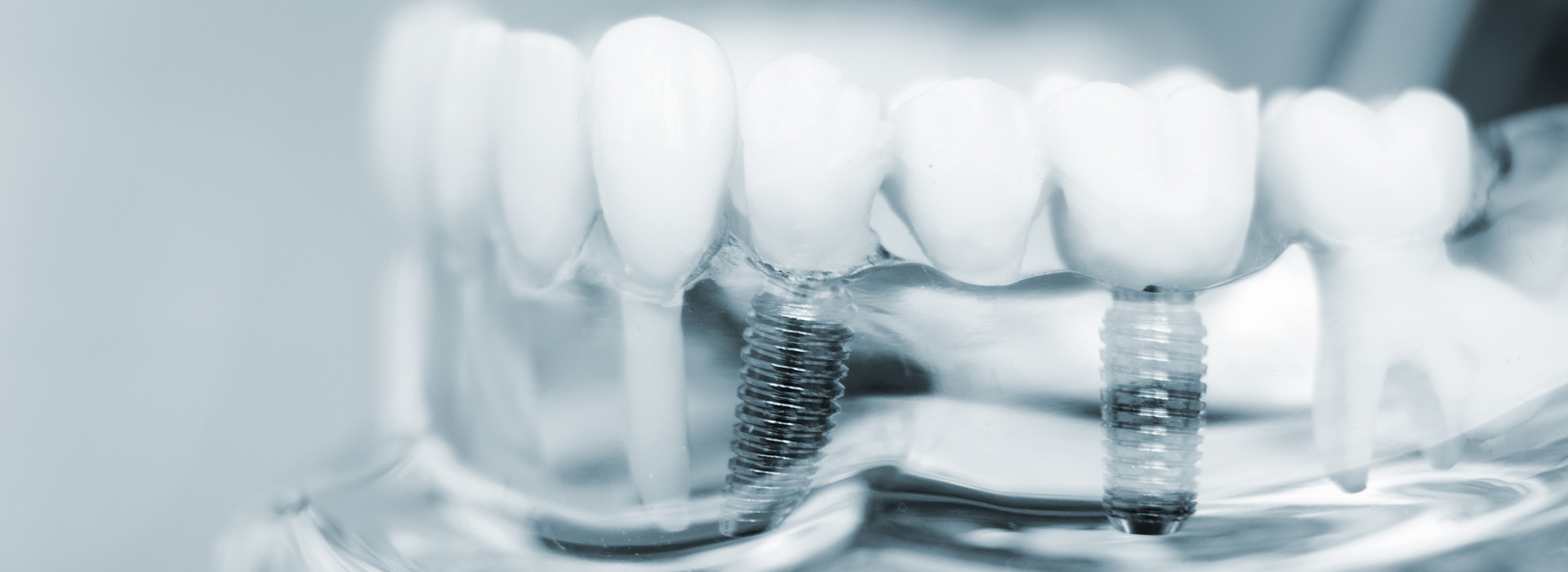
A dental implant begins with a small titanium post placed in the jawbone where a tooth root once was. Over the following months, that post fuses to the bone through a biological process called osseointegration, creating a stable anchor. Once integration is complete, a custom-made crown, bridge, or denture is attached to that foundation, restoring the visible portion of the tooth while the implant provides the underlying support.
Because implants replace the root as well as the crown, they preserve the bone by transmitting chewing forces down into the jaw. This stimulation helps maintain facial contours and prevents the gradual bone loss that typically follows tooth extraction. The result is a restoration that looks and functions much more like a natural tooth than traditional removable options.
Patients often notice improved comfort and function compared with dentures and better long-term oral health compared with bridges that rely on neighboring teeth. With routine care and proper planning, implants can be a reliable, long-lasting element of modern restorative dentistry.
A complete implant restoration has three essential components: the implant (the surgical post), the abutment (the connector), and the prosthesis (crown, bridge, or denture). Each piece is designed to work together so the restoration is stable, hygienic, and lifelike. The implant provides the structural support, the abutment positions the restoration above the gum line, and the prosthesis recreates the tooth’s form and function.
Modern materials and CAD/CAM technologies allow the prosthetic portion to be custom-shaped and color-matched for a seamless appearance next to natural teeth. Precision in these stages — accurate implant placement, precise impressions or digital scans, and careful lab work — is what produces predictable, natural-looking results.
Determining candidacy for implants starts with a comprehensive exam that includes clinical assessment and three-dimensional imaging. We evaluate jawbone volume, the health of surrounding teeth and gums, bite relationships, and overall medical history. This information helps us create a tailored plan that considers both immediate needs and long-term wellness.
In some cases, preparatory procedures such as bone grafting or tooth extractions may be needed to create an optimal environment for implant placement. We discuss these options openly and plan each step to minimize discomfort and maximize the chance of a successful outcome.
One of the most immediate advantages of implants is the return of reliable chewing ability. Because implants are anchored to the jawbone, they resist the shifting and movement experienced by some removable options. This stability makes it easier to enjoy a normal diet and reduces limitations many people feel with traditional dentures.
Speech can also improve. Ill-fitting removable prostheses may introduce slurring or clicking, whereas fixed implant restorations maintain consistent positioning, helping patients speak naturally and confidently. Comfort increases as the implant becomes integrated and the restoration sits precisely where it should, eliminating the friction and sore spots associated with poor-fitting dentures.
Beyond daily convenience, implants offer oral-health benefits: they preserve surrounding bone, protect neighboring teeth from unnecessary preparation, and create restorations that are easy to clean. Unlike conventional bridges that require altering adjacent teeth, implants support prostheses without compromising healthy tooth structure.
Because implants are made of materials that do not decay, they eliminate the risk of cavities in the replaced tooth. With good oral hygiene and regular dental care, an implant-supported restoration can remain a dependable solution for many years.
Preparation begins with a detailed discussion of goals and a thorough exam. Digital imaging and models help us visualize the bone and plan ideal implant positions. If bone volume is insufficient, a graft may be recommended to create a stable foundation. These preparatory steps are designed to reduce surprises and improve long-term predictability.
We also review options for anesthesia and comfort during treatment. Many implant procedures are performed on an outpatient basis with local anesthesia and, when appropriate, conscious sedation to keep patients relaxed. Clear pre-operative instructions and answers to questions are an important part of our approach to patient-centered care.
Implant surgery is generally considered a routine outpatient procedure. After placement, a healing period allows the implant to integrate with the bone — a process that typically takes several months. During that time, temporary restorations can be used so patients do not go without teeth.
Once healing is complete, the final prosthetic components are attached and adjusted for comfort and function. Long-term success depends on daily oral hygiene, routine dental visits, and managing risk factors such as gum disease. With proper care, many implant restorations provide durable, satisfying results for years to come.
Bone grafting is a common adjunctive procedure when the jaw lacks sufficient volume for ideal implant placement. Grafting rebuilds lost bone so an implant can be positioned in the proper location and angle, which is critical for both longevity and appearance. Techniques vary depending on the extent of bone loss, and many grafts integrate predictably when placed by experienced clinicians.
We evaluate each case individually and explain why a graft may be recommended, what materials are used, and the expected healing timeline. Thoughtful planning and careful execution of grafting procedures increase the likelihood of successful implant integration and a stable result.
Dental implants offer a flexible, long-term solution for replacing missing teeth, restoring not only appearance but the function and health of the jaw. Whether you need a single crown, an implant-supported bridge, or a full-arch reconstruction, careful planning and skilled execution are the keys to predictable, natural-looking outcomes.
If you’d like to learn more about how implants could work for your smile, contact Vita Head, Neck & Facial Pain Relief Center for a consultation. Our team will review your options, answer your questions, and outline a personalized treatment plan tailored to your needs.

If you've lost a tooth due to injury, decay, gum disease, or any other reason, we recommend dental implants to replace missing teeth. Dental implants come the closest to replicating the look, feel, and function of your natural teeth.
Dental implants are placed into the jawbone and mirror the same function as the root of a tooth. The procedure for dental implants is usually performed while a patient is sedated. Patients who undergo IV sedation must have an empty stomach and transportation home following the procedure. Most sedation patients will have little to no memory of the procedure occurring.
Generally, dental implants are made out of a biocompatible metal such as titanium. Biocompatible metals are also used for other common bone implants (such as shoulder, hip, and knee replacements). The visible portion of the implant is usually made out of porcelain and is custom-made to match your existing teeth.
Dental implants are designed to fuse to the bone, which makes them become permanent fixtures. Typically speaking, the success rate is nearly 100%. There are few cases in which the implant will not fuse as intended and must be removed. If this happens to occur, the procedure can be attempted again a few months later.
Dental implants are not usually covered by dental insurance, but may be covered under a patient's medical insurance. Our office and your insurance company can discuss coverage options with you based on your individual case and treatment plan.
It's easy... just take care of an implant as if it's a natural tooth! This involves regular brushing, flossing, and dental checkups. If you have any concerns about your implant, contact us immediately.
Implant dentistry replaces missing teeth by restoring both the root and the visible crown rather than relying on removable appliances or adjacent teeth for support. A small titanium post is placed in the jawbone to act as a stable anchor that integrates with bone through osseointegration. Once integrated, a custom-made abutment and prosthesis restore appearance and function.
This approach preserves jawbone volume and facial contours by transmitting chewing forces into the bone, which helps prevent the bone loss that follows extraction. Implants can be used for single teeth, multiple missing teeth, or full-arch reconstructions, offering options that fit a range of functional and aesthetic needs. With careful planning and follow-up care, implants provide a durable foundation for lifelike restorations.
A dental implant system includes a surgically placed titanium post, an abutment that connects the post to the prosthesis, and the crown, bridge, or denture that recreates the tooth. The titanium post fuses with the jawbone over time, creating a stable base similar to a natural tooth root. The prosthetic portion is custom-shaped and color-matched to blend with adjacent teeth.
Because implants replace the root and restore the crown, they transmit chewing forces into the bone and help maintain bone health and facial structure. Patients typically experience improved chewing efficiency and more consistent speech compared with ill-fitting removable options. Proper prosthetic design and precise placement are critical to achieving a comfortable, natural-feeling result.
Candidates are evaluated on overall health, oral health, and sufficient jawbone volume to support an implant. Healthy gums, controlled chronic conditions, and a commitment to oral hygiene are important factors in candidacy. Smoking and certain medications can affect healing and are discussed during the evaluation.
Three-dimensional imaging and a clinical exam allow clinicians to assess bone quality, nerve location, and sinus position to determine the best approach. When bone is inadequate, preparatory procedures such as bone grafting or sinus lifts can often create a suitable foundation for implants. Your care team will outline these options and a timeline so you understand what to expect before placement.
The process begins with a consultation that includes a thorough dental exam, medical history review, and detailed imaging to map bone and surrounding structures. Digital planning tools help determine ideal implant positions and whether adjunctive procedures are needed. A personalized treatment plan is created to address function, aesthetics, and timing.
Implant placement is typically performed as an outpatient procedure with local anesthesia and, when appropriate, conscious sedation to keep patients comfortable. The implant post is surgically positioned in the bone, and temporary restorations are used when needed so patients do not go without teeth. Pain is usually manageable with prescribed or over-the-counter medication and guided post-operative instructions.
After placement a healing period allows the implant to integrate with bone, and follow-up visits monitor progress and soft-tissue healing. Once integration is stable, the abutment and final prosthesis are attached and adjusted for bite and comfort. Long-term success depends on routine oral hygiene, regular professional care, and managing risk factors such as periodontal disease.
Healing and integration of an implant commonly take several months, though timelines vary based on individual biology and the specific treatment plan. In some cases, immediate or early loading allows temporary or definitive teeth to be placed sooner, while other situations require staged healing to protect the implant. Factors such as bone quality, the need for grafting, and systemic health influence the overall schedule.
Your clinician will outline expected milestones, including dates for placement, provisional restorations, and the delivery of the final prosthesis. Regular follow-up appointments are scheduled to confirm osseointegration and to make any necessary adjustments to fit and function. Clear communication about expectations helps patients plan for recovery and return to normal diet and activities.
Single-tooth implants support an individual crown without affecting adjacent teeth, preserving healthy tooth structure. For several missing teeth in a row, implant-supported bridges use implants as anchors rather than relying on natural teeth for support. These approaches help maintain bone and deliver predictable chewing function.
For full-arch replacement, fixed prostheses supported by four to six implants can restore a non-removable set of teeth that closely mimic natural dentition. Implant-retained overdentures offer a removable option that snaps onto implants for greatly improved stability over conventional dentures. Choice of restoration depends on anatomy, patient preference, and functional goals discussed during planning.
Complications can include infection, failed integration, damage to nearby structures such as nerves or sinuses, and peri-implant inflammation around the implant site. Careful planning with three-dimensional imaging and precise surgical technique reduce many of these risks. Early detection through routine follow-up allows timely management when issues arise.
Treatment for complications may include professional cleaning, antibiotics, modification of the prosthesis, or, in rare cases, removal and replacement of the implant. Addressing contributing factors such as uncontrolled periodontal disease or smoking is an important part of preventing recurrence. Your treatment team will explain signs to watch for and a management plan tailored to your situation.
Daily brushing and interdental cleaning with floss or interdental brushes are essential to remove plaque and protect the tissues around implants. Professional cleanings and periodic evaluations allow clinicians to check for signs of inflammation, prosthetic wear, or bite changes. Lifestyle choices such as smoking cessation and managing conditions that affect healing support implant longevity.
For patients who grind or clench teeth, a nightguard can protect both natural teeth and implant restorations from excessive forces. Maintain regular appointments so occlusion and prosthetic components can be adjusted before small issues become larger problems. With consistent home care and professional oversight, implants can remain functional and healthy for many years.
Bone grafting or sinus augmentation is often recommended when jawbone volume or quality is insufficient to support an implant in the ideal position. Grafting materials and techniques vary from small particulate grafts to block grafts or specialized membranes depending on the site and amount of augmentation needed. These procedures rebuild a stable foundation so implants can be positioned for both long-term function and aesthetic outcomes.
Healing times after grafting vary but are typically several months before implant placement to allow the graft to integrate with native bone. In some situations, implants can be placed at the same time as grafting, while other cases require staged treatment for predictability. Your clinician will recommend the most appropriate approach based on imaging, clinical findings, and treatment goals.
Restorations that restore proper tooth height, alignment, and occlusion can have a positive effect on jaw function and may reduce strain that contributes to TMJ discomfort. Because implant-supported restorations are rigidly anchored, careful occlusal design is required to distribute forces evenly and avoid creating new imbalances. Evaluation by clinicians experienced in facial pain and neuromuscular relationships helps integrate implant therapy with TMJ care when indicated.
At Vita Head, Neck & Facial Pain Relief Center we coordinate implant planning with a broader assessment of jaw function to ensure restorative work supports long-term comfort and function. This collaborative approach includes thorough examination, imaging, and discussion of treatment sequencing so implants complement other therapies for facial pain or headache issues. Patients are encouraged to discuss symptoms of jaw pain or headaches during the implant consultation so the treatment plan addresses the whole-person needs.

We’re here to answer your questions and help you take the next step toward relief.
Have questions about your symptoms, treatment options, or scheduling an appointment? Our friendly and knowledgeable team is always happy to assist you. Whether you’re seeking relief from TMJ disorders, head and neck pain, facial discomfort, or general dental concerns, we take the time to listen and provide clear, thoughtful answers. From your first call to your ongoing care, we are committed to offering personalized support, helping you understand your options, and guiding you toward lasting comfort, improved function, and exceptional care.